 |
|||
|
|
|||
|
 |
 |
|||||
|
|
||||||
|
What is Breast Thermography
|
||||||||
|
Breast thermography is a diagnostic imaging procedure that helps you in the early detection of breast cancer.
State-of-the-art breast thermography uses an ultra-sensitive infrared medical camera combined with a sophisticated computer program. This system produces high-resolution diagnostic images of these temperature and vascular patterns of the breast. These images are then analyzed by our Certified Thermologist. The procedure is both comfortable and safe using no radiation or compression. By carefully examining changes in the temperature and blood vessels of the breasts, signs of possible cancer or pre-cancerous cell growth may be detected up to 10 years prior to being discovered using any other procedure. These temperature variations and vascular changes may be among the earliest signs of breast cancer and/or a pre-cancerous state of the breast.(3,6,7,8,9). Breast thermography's ability to detect a pre-cancerous state of the breast, or signs of cancer at an extremely early stage, lies in its unique capability of monitoring the temperature variations and blood vessel alterations produced by the earliest changes in tissue physiology (function).(3,6,7,8,9) Breast thermography has been researched for over 30 years, and over 800 peer-reviewed breast thermography studies exist in the index-medicus. In this database, over 250,000 women have been included as study participants. Some of these studies have followed patients up to 12 years. The research has shown that breast thermography has an average sensitivity and specificity of 90%.
Studies show that:
Just as unique as a fingerprint, each patient has a particular infrared map of their breasts. Any modification of this infrared map on serial imaging (images taken over months to years) can constitute an early sign of an abnormality. In patients without cancer, the examination results are used to indicate the level of possible future cancer risk(4,5). Consequently, in the absence of other positive tests, an abnormal infrared image gives a woman an early warning. By maintaining close monitoring of her breast health with serial infrared imaging, self breast exams, clinical examinations, and other tests, a woman or man has a much better chance of detecting cancer at its earliest stage and preventing invasive tumor growth. A positive infrared scan may indicate the presence of many different breast abnormalities such as mastitis, fibrocystic breast disease, cancer, hormone imbalances (excessive estrogen in the breast), and others. However, thermography does not have the ability to pinpoint the location of a tumor. Consequently, breast thermography's role is in addition to mammography and physical examination, not in lieu of. Breast thermography does not replace mammography and mammography does not replace breast thermography, the tests complement each other. Since it has been determined that 1 in 8 women will get breast cancer, we must use every means possible to detect cancers when there is the greatest chance for survival (1). Proper use of breast self-exams, physician exams, thermography, and mammography together provide the earliest detection system available to date(3,7,8,9). If treated in the earliest stages, cure rates greater than 95% are possible(3,6). The addition of breast thermography to the frontline of early breast cancer detection brings earlier detection and a greater chance of survival. Click here to go to Understanding your risk rating. Thermogram Test:
References
|
||||||||
|
|

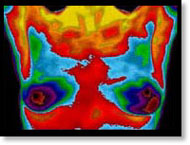 The procedure is based on the principle that chemical and blood vessel activity in both pre-cancerous tissue and the area surrounding a developing breast cancer is higher than in a normal breast. Since pre-cancerous and cancerous masses are highly metabolic tissues, they need an abundant supply of nutrients to maintain their growth. In order to do this, they increase circulation to their cells by sending out chemicals to keep existing blood vessels open, recruit dormant vessels, and create new ones (neoangiogenesis). This process results in an increase in regional surface temperatures of the
The procedure is based on the principle that chemical and blood vessel activity in both pre-cancerous tissue and the area surrounding a developing breast cancer is higher than in a normal breast. Since pre-cancerous and cancerous masses are highly metabolic tissues, they need an abundant supply of nutrients to maintain their growth. In order to do this, they increase circulation to their cells by sending out chemicals to keep existing blood vessels open, recruit dormant vessels, and create new ones (neoangiogenesis). This process results in an increase in regional surface temperatures of the